If you have a rare form of psoriasis, it can seem like plaque psoriasis gets all the attention.
All those TV ads for psoriasis treatments are for plaque psoriasis. Kim Kardashian tweets about her . . . plaque psoriasis. And invariably, when a new treatment is FDA-approved, it is for plaque psoriasis.
Perhaps that is understandable, given that 80%-90% of people with psoriasis have plaque psoriasis, though some people have more than one kind. But it can make things challenging when looking for a treatment to help you.
The treatments prescribed for inverse, guttate, pustular, and erythrodermic psoriasis are typically “off label,” which means a physician is prescribing, for those types of psoriasis, a drug that the US Food and Drug Administration (FDA) approved for a different use. Many off-label uses are universally accepted – for example, methotrexate being used for psoriatic arthritis. But off-label use also adds more art to the art and science of selecting psoriasis treatments.
What follows is an introduction to some of the treatments considered for these less common, but extremely distressing, types of psoriasis. Clinical trials for these types of psoriasis are rare, so much of the discussion below has developed from treatment ideas passed along doctor to doctor and eventually made public, or through “case studies” published in scientific journals about one or a few specific people. Evidence like this is not as strong as that gleaned from clinical trials, but accumulated wisdom is very much still worth knowing.
And we would note, again, a piece of advice we give frequently, which is particularly true when dealing with less common psoriasis subtypes: if selecting a new dermatologist, try to find one who treats multiple patients with your psoriasis type. All physicians can learn the science of medicine, but the art is typically learned over time and through trial and error.
Inverse Psoriasis
Inverse psoriasis is also known as intertriginous psoriasis. It appears as red lesions (often more purple or brown in darker skin, or a deeper red), sometimes smooth and shiny, in body folds — armpits, underneath the breasts, around the genitals and buttocks. Lesions can bleed and cause painful cracks — known as fissures — in creases of your skin. It can be linked to yeast, fungal, and bacterial infections. Unlike plaque psoriasis, inverse psoriasis is often moist; though just like other psoriasis, it can sting, itch, or both. Even though inverse psoriasis may be a small fraction of a person’s total area of skin, it can be extremely unpleasant and demoralizing.
Inverse psoriasis is more common in people who are obese and who have deep skin folds, where rubbing and sweating occur. You can have inverse psoriasis and also have another type of psoriasis on your body as well.
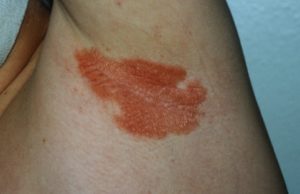
Inverse psoriasis can be confused with “jock itch,” a fungus that starts with irritation between your thigh and groin. Jock itch can spread and blister; your skin may get flaky or scaly, and it may itch or burn. Jock itch can be treated with antifungal creams.
Try to keep inverse psoriasis cool and dry. Natural fibers like cotton might help reduce irritation and let the skin “breathe.” Minimizing friction – though that can be hard to do – can also help.
Inverse psoriasis is often treated with topical creams, though more serious cases may be addressed with ultraviolet night (UVB), biologic treatment, or pills that work on the entire body. (Taltz is one biologic that has shown success treating inverse psoriasis.)
Corticosteroids (often called topical steroids). This is often the first class of medicines prescribed, and may come as a cream, ointment, foam, oil, gel, spray, or foam. You’ll need to be careful to follow usage instructions carefully, since overuse can lead to stretch marks or make thin skin in affected areas even thinner. Generally, the milder topical steroids are used on inverse psoriasis, though more potent options can be used in very short courses. If you also have a yeast or fungal infection, treatments for those conditions may be combined with corticosteroid treatment.
Dovonex (calcipotriene). This is a synthetic form of vitamin D, and slows the growth and development of skin cells. Side effects may include a feeling of stinging or burning. This can be used with topical steroids to reduce the amount of steroid needed, allowing for long-term use while minimizing potential side effects.
Elidel Cream (pimecrolimus) and Protopic ointment (tacrolimus). These non-steroidal treatments were FDA-approved for atopic dermatitis (eczema), another skin condition. But physicians report they have had success treating inverse psoriasis with these medications. They are typically prescribed for short-term use, as some studies link these treatments to a slight increase in cancer risk. They can also be used in conjunction with topical steroids.
Castellani’s Paint (Castederm and others). This medication is prescribed to dry psoriasis lesions in skin folds when doctors believe you may also have a bacterial or fungal infection. Other drying agents include baby powder, baking soda, and zinc oxide powder.
Don’t let embarrassment about inverse psoriasis’ placement on your body deter you from receiving treatment for it. Doctors have seen it all, and there are treatments that can give you tremendous relief from the pain and other symptoms of this nasty psoriasis subtype. Get it treated!
Guttate Psoriasis
Guttate psoriasis is the second most common form of psoriasis. It appears, often suddenly, as many small, red (though it can appear closer to purple or brown in darker skin, or a deeper red), scaly, droplet-shaped bumps, usually covering the trunk, arms, and legs, though they can appear anywhere. Guttate psoriasis lesions — known as “papules” — are not as thick as lesions from plaque psoriasis. It is possible to have both types at the same time.
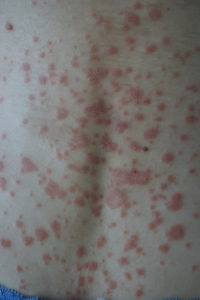
Guttate psoriasis is usually diagnosed in children or young adults, and can be genetic — if someone in your family has it, you may develop it too. It is frequently triggered by strep throat, or other infections. Anti-malarial medicines and beta-blockers have also been cited as triggers.
Guttate psoriasis flares can go away on their own, typically after 2-3 weeks, though in other case a few months. But there are treatments used to hasten clearance.
Despite guttate psoriasis being relatively common, there is surprisingly little research specifically on guttate psoriasis treatments. Back in 2000, one comprehensive review up to that date found not a single credible study evaluating guttate psoriasis treatments. While the situation is not much better today, we do have extensive real-world experience treating guttate flares, and the medical community uses much of the plaque psoriasis arsenal of treatments that have been found to work on guttate psoriasis.
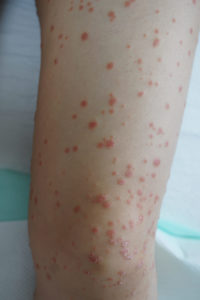 Your doctor may prescribe topical steroid creams, light (UVB) therapy (or actual sunlight), and/or oral medications for guttate psoriasis. Because guttate psoriasis can be so widespread, topical steroids may be impractical or unwise, since excessive topical steroid use can cause significant side effects. If a bacterial infection triggered the condition, antibiotics may be prescribed as well. If guttate psoriasis resists the first lines of treatment, your doctor may suggest a biologic treatment. It should be noted that pregnant women with guttate psoriasis can safely be treated with UVB.
Your doctor may prescribe topical steroid creams, light (UVB) therapy (or actual sunlight), and/or oral medications for guttate psoriasis. Because guttate psoriasis can be so widespread, topical steroids may be impractical or unwise, since excessive topical steroid use can cause significant side effects. If a bacterial infection triggered the condition, antibiotics may be prescribed as well. If guttate psoriasis resists the first lines of treatment, your doctor may suggest a biologic treatment. It should be noted that pregnant women with guttate psoriasis can safely be treated with UVB.
Guttate psoriasis is rather unpredictable. Often, once the strep throat or other infection is cleared, the guttate flare dissipates as well, and may never return. However, in other cases, it can become chronic, or turn into plaque psoriasis, or reappear many years later.
Pustular Psoriasis
Pustular psoriasis appears as red skin surrounding white bumps — “pustules” — filled with pus. The pus is made up of white blood cells; it is not an infection and is not contagious. The pustules may hurt or itch and may be flaky or scaly. This condition can run in families, though it most commonly appears in adults, not children.
Pustular psoriasis can have various triggers, including overexposure to UV light (sunlight), pregnancy, infections, and sudden discontinuance of topical or systemic treatments, particularly prednisone and other systemic corticosteroids.
There are several forms of pustular psoriasis, classified by where and how quickly the pustules appear:
Palmoplantar pustulosis (PPP): Pustules form on the palms of the hand, soles of the feet, or other small areas of the body — the base of the thumb and sides of the heels are commonly affected. Its placement on the hands and feet makes it particularly painful and debilitating. This type of psoriasis often occurs in cycles, with fresh pustules starting red with white pus, then turning brown and peeling off or forming a crust, sometimes leading to cracked skin. Smoking tobacco is considered one of the major triggers, another being infections.
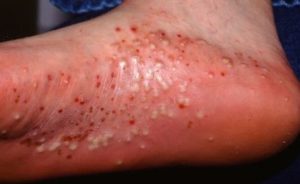
Some biologic TNF-alpha inhibitors are believed to trigger a PPP flare in rare cases; ironically, one of the TNF-alpha inhibitors, Enbrel, has been proposed as an effective treatment for biologic-induced PPP flares. Another is a different kind of biologic, Actemra (tocilizumab).
In 2019, results of a rare clinical trial in PPP were announced, with 159 PPP patients, demonstrating that the biologic Tremfya showed significant improvement of PPP symptoms after 16 weeks, with benefits being visible after 8 weeks. (For those with PPP, just having a clinical trial done on their behalf is a big step forward; treatment decisions for pustular psoriasis are generally made based on trial and error and theories, rather than full-blown clinical trials.)
UV light treatments (phototherapy) may be used for PPP and acropustulosis (see below). A combination of Soriatane plus PUVA has shown success in treating PPP (although women of child bearing potential should try to avoid Soriatane). Cyclosporine and Stelara are other options. (In a very small – 5 patient – test of Stelara for PPP, all five started to improve after 3 weeks, and all had “complete or nearly complete resolution of lesions and a significant improvement in patients’ quality of life” at week 20.) Direct application of topical steroids and other agents to the palms and soles is also done. PPP lacks a gold standard treatment, but most plaque psoriasis treatments can provide some measure of relief from PPP flares.
Acropustulosis: This is an uncommon form of psoriasis in which painful lesions develop on fingertips or toes, making it painful to move or use the affected areas. Acropustulosis can damage nails and, in rare acute cases, damage bones as well.
Generalized (Von Zumbusch): This is a rare, serious form of psoriasis that mostly affects adults. It requires immediate medical attention and can be life-threatening. Red, painful blotches develop quickly all over the body, followed within hours by blisters filled with pus (pustules). The patient may also have itchy skin, fatigue, pain, and have symptoms of fever — chills, dehydration, nausea, muscle weakness, headache, joint pain, and/or racing pulse. Pustules will dry and peel off within 1-2 days, and affected skin will appear glazed. The process can then repeat itself.
A generalized pustular outbreak requires immediate medical attention. Doctors will check blood calcium levels, which can become dangerously low, give the patient fluids to prevent dehydration, and treatment against fever and infection. Hospitalization is not uncommon during these flares.
A generalized outbreak can be treated with fast-acting medications like cyclosporine or Remicade. Other treatment options include Soriatane, methotrexate, or biologics such as Enbrel, Stelara, Cosentyx, or Taltz. There are indications that another biologic, Kineret (anakinra), may also be effective. After the immediate crisis is controlled, treatment with ultraviolet (UV) light directed at affected areas becomes an option.
A few reports indicate that Remicade and cyclosporine have been used successfully in treating pustular psoriasis in pregnancy.
Among the complications that can occur with generalized pustular psoriasis are respiratory distress, liver damage, bacterial skin infections, and malnutrition. The risk of dying from generalized pustular psoriasis is higher in the elderly and in those who do not get treated during an acute outbreak.
Pustular psoriasis is best treated by dermatologists who treat many psoriasis patients, who thus have familiarity with the widest range of possible treatments.
Erythrodermic Psoriasis
Erythrodermic psoriasis is a rare, potentially life-threatening form of psoriasis that requires immediate medical attention. The main symptom of erythrodermic psoriasis is fiery red skin all over the body; it can develop over time or come on quickly. Skin comes off in large sheets, not scales, and looks as if it has been burned. Heart rate may increase and body temperature may fluctuate, resulting in chills or fever. Swelling may develop from retained fluid, especially around the ankles. Because the skin system has been compromised, the body can lose proteins and fluids and have trouble fighting off infections. Erythrodermic psoriasis can lead to pneumonia, sepsis, or congestive heart failure.
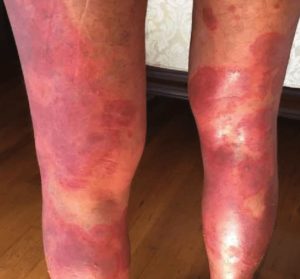
Triggers for erythrodermic psoriasis can include sudden withdrawal of oral steroids like prednisone, untreated severe psoriasis, severe sunburn, and infections. Most people who develop erythrodermic psoriasis already have another type of psoriasis. Before developing erythrodermic psoriasis, they often notice that their psoriasis is worsening or not improving with treatment.
Hospitalization is common with erythrodermic flares. Doctors may need to provide IV fluids to prevent dehydration, and antibiotics to combat infection. Cyclosporine and the biologic Remicade are considered good agents to try to hit an erythrodermic flare hard. Soriatane is another good option (although not good for women of childbearing potential). Other biologics with rapid onset of benefit, including Taltz and Cosentyx, also show promise in combatting erythrodermic psoriasis flares, as do the biologics Enbrel, Stelara, and Simponi.
Unfortunately, research on treating erythrodermic psoriasis is very limited, leading to a reliance on single case reports and other anecdotal evidence to craft treatment protocols. About 3% of psoriasis patients have erythrodermic psoriasis.
Erythrodermic psoriasis should be treated by a dermatologist with demonstrated expertise in treating severe psoriasis.
Conclusion
While we need more research targeted to rare psoriasis subtypes, the good news is that the biologics approved for plaque psoriasis, as well as some other biologics, are also proving effective in improving the symptoms of the hard-to-treat subtypes. This should give us all reason to be hopeful that brighter days are finally ahead for people battling these difficult conditions.
[Last updated 6-9-2020]


