Diagnosing and Understanding Psoriatic Arthritis
ARTICLE SUMMARY: Psoriatic arthritis is a form of arthritis often seen in psoriasis patients. It causes joint pain, swelling, and stiffness. Left untreated, it can cause permanent damage. So seeking diagnosis and treatment of psoriatic arthritis is very important.
Click here to go directly to Treatments for Psoriasis and Psoriatic Arthritis.
Psoriatic arthritis, as its name suggests, is a form of arthritis that is closely associated with the disease psoriasis. Like other forms of arthritis, psoriatic arthritis (PsA) causes pain, swelling, and stiffness of the joints. The fingers, toes, and spine are common trouble spots. Over time, PsA can damage and deform affected joints, interfering with joint function. Changes in the nails are another hallmark of psoriatic arthritis, and fatigue is a frequent symptom.
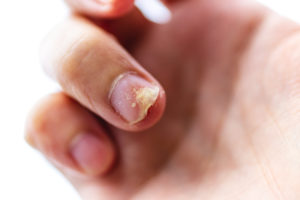
Most people who develop PsA have been living with the skin symptoms of psoriasis for years; however, in some cases psoriatic arthritis manifests itself in the joints at the same time as, or even before, psoriasis appears on the skin. Efforts to determine how often PsA occurs among psoriasis patients have produced widely varying results — but it appears roughly 1 in 4 psoriasis patients will develop PsA.
PsA is a serious matter. More than three-quarters of psoriatic arthritis patients in a major international survey reported moderate to severe disease. And nearly one-third of those psoriatic arthritis patients reported that PsA had impacted their ability to work full time. A 2019 study of psoriatic arthritis patients in Denmark found that 29% required joint surgery by 15 years after their initial diagnosis, compared to 14.6% of the general population.
Diagnosing psoriatic arthritis
Not everyone who has psoriasis and arthritis has PsA. People with psoriasis can develop other types of arthritis, such as rheumatoid arthritis (RA) and osteoarthritis (OA), just like anyone else in the general population. Therefore, doctors must delve into the details of arthritic symptoms in psoriasis patients in order to correctly diagnose PsA and recommend optimal treatment.
Characteristics of psoriatic arthritis
The joint pain and swelling of psoriatic arthritis is believed to be caused by the overactive inflammation that people with psoriatic arthritis have internally, impacting their immune system. Other psoriasis symptoms, such as skin plaques and nail disease, likely have the same underlying immunological cause.
 Some other common features of PsA include: arthritis of the joints nearest the tips of the fingers and toes, arthritis of the spine, inflammation of tendons and ligaments at the sites of attachment to the bones (enthesitis), and inflammation / swelling of one or more fingers or toes (dactylitis or “sausage digits”). When a joint on one side of the body is involved, the corresponding joint on the other side is not necessarily involved, a so-called asymmetric distribution of disease.
Some other common features of PsA include: arthritis of the joints nearest the tips of the fingers and toes, arthritis of the spine, inflammation of tendons and ligaments at the sites of attachment to the bones (enthesitis), and inflammation / swelling of one or more fingers or toes (dactylitis or “sausage digits”). When a joint on one side of the body is involved, the corresponding joint on the other side is not necessarily involved, a so-called asymmetric distribution of disease.
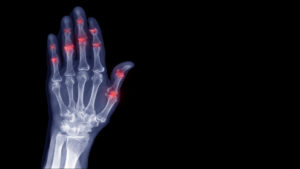
X-ray or other imaging studies of PsA-affected joints can reveal erosion of bone, narrowing of the space inside the joint, and fusion of adjacent bones. Like psoriasis itself, psoriatic arthritis can be mild, moderate or severe; however, PsA can cause significant structural damage to the joints even in cases when pain and other external symptoms are relatively mild.
PsA affects men and women in equal numbers. Finally, rheumatoid factor, a molecule found in the blood of most people with rheumatoid arthritis, is only rarely present in those with psoriatic arthritis.
Differences between psoriatic arthritis and other types of arthritis
Rheumatoid arthritis is also an inflammatory, immune-based arthritis and shares many similarities with psoriatic arthritis. In fact, both diseases respond to many of the same medications, especially methotrexate and the biologic therapies that target the immune system. Two or three percent of patients with RA have psoriasis (about the same as the frequency of psoriasis in the general population), so there is potential for confusion of the two conditions. Unlike PsA, however, RA is nearly always associated with rheumatoid factor in the blood. Also, patients with RA are less likely to have back pain, enthesitis, and dactylitis, and are more likely to have a symmetrical distribution of arthritic joints.
Osteoarthritis occurs when the protective cartilage inside joints is damaged or worn away by years of use. OA is extremely common in older people—60% of people aged 65 or older have symptoms of OA—so statistically speaking, an older person with psoriasis and arthritis is more likely to have OA than PsA. Some features of OA and PsA overlap. The affected joints are usually asymmetrically distributed, and the finger and toe joints are often involved. However, patients with OA do not normally have spinal arthritis, enthesitis, or dactylitis, and many of the abnormalities seen in X-rays of PsA-affected joints, such as fusion of bones within the joint, are uncommon in OA. Because treatments available for the two conditions differ, it is important to accurately distinguish between them. For example, the biologic therapies that can produce dramatic improvements in PsA are not used to treat OA.
Treatment of psoriatic arthritis
Treatment of psoriatic arthritis is important, and can be quite effective in relieving painful symptoms. In addition, newer treatments for PsA have been shown to stop the progression of joint damage. But no treatments have yet been shown to reverse damage that has already occurred. For that reason alone, if you suspect you might have psoriatic arthritis, you should get yourself to a rheumatologist (a specialist in arthritis), or, at a minimum, a dermatologist knowledgeable about psoriasis.
Further reading: Psoriasis and psoriatic arthritis treatment options.
[Last updated 5-25-2020]


