Psoriasis is an inflammatory disease involving the immune system that can first strike at any age, causing dry, painful skin lesions that itch, crack, and can bleed.
Psoriasis is not contagious, although it is generally persistent or recurring, with as many as 7.5 million Americans affected, according to the U.S. National Institutes of Health.
While psoriasis has long been known as a skin disease, it is actually an internal, system-wide disease of the body, in which an overactive immune system leads to inflammation, triggered by some combination of genetics and many other factors in someone’s life. While the skin symptoms are what you see, psoriasis can increase the likelihood of a wide range of other conditions and diseases, most commonly psoriatic arthritis, a chronic, progressive and potentially debilitating disease that causes painful joint inflammation, stiffness, and tenderness, and that can damage bones. Other diseases that are more common in psoriasis patients than in people who do not have psoriasis reads like a laundry list of major health issues, including heart disease, high blood pressure, type 2 (adult onset) diabetes, depression, Crohn’s disease, and obesity.
(If you or a loved one has been recently diagnosed with psoriasis, the previous paragraph probably freaked you out. If you read on, you will learn that it is not as bad as it sounds. We’re simply laying out the facts before we get to the good news. But you should probably go directly to Newly Diagnosed, our home page for those who are still processing the news of their psoriasis diagnosis, where we give you key introductory information and strategies for how to proceed.)
Fortunately, for most people with psoriasis, the disease is mild. They might have patches of dry skin on their elbows or knees and be able to treat it with over-the-counter or prescription creams and lotions.
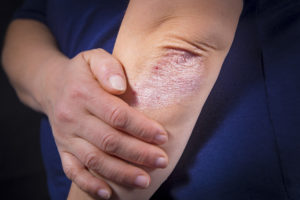
Still, for millions of other Americans, psoriasis is a daily impediment, one that dramatically and negatively impacts their quality of life. For many, it is debilitating. A National Institute of Mental Health-sponsored study in the Journal of the American Academy of Dermatology found that “Patients with psoriasis reported reduction in physical functioning and mental functioning comparable to that seen in cancer, arthritis, hypertension, heart disease, diabetes, and depression.” Psoriasis hurts. Psoriasis itches. Some people have extensive coverage—on their arms, legs, trunk, scalp, face, and/or genitals. [Read more about scalp psoriasis and its treatments.]
But what is striking and even less well known is how devastating psoriasis can be emotionally and psychologically. It is not just a disease that harms the body. Psoriasis patients have a higher incidence of depression, and even of suicidal thoughts. The visible nature of psoriasis exacerbates its interference with intimacy and one’s sense of self. Self-esteem can take a hit.
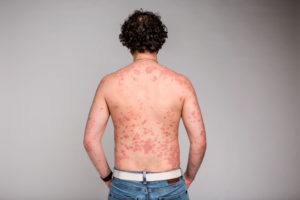
An increasing number of genes are being identified as playing a role in making someone susceptible to psoriasis, which is why psoriasis can run in families. But other factors are also involved. Skin injury and infections—like strep throat—are the most common environmental factors that can trigger psoriasis flares. Stress is also widely believed to play a role (though the actual studies looking for the causal link are somewhat lacking, and we find the constant focus on stress, and anecdotes about “trigger foods,” overplayed and perhaps counterproductive). Diet does not appear to play a significant role in the disease, although obesity is more common among psoriasis patients than the general public, and appears to make psoriasis worse.
Overuse of alcohol and tobacco are associated with psoriasis, but figuring out cause and effect is difficult and not yet resolved. Some experts believe people with psoriasis turn to these things to deal with the trauma of psoriasis, while others believe excessive alcohol or tobacco can trigger psoriasis. Both theories may prove true. People with psoriasis should certainly seek to control their consumption of alcohol and tobacco, even for reasons other than psoriasis.
In normal skin, it takes about a month for skin cells to move from the bottom layer to the surface and slough off unnoticed in a continuous cycle. But in skin affected by psoriasis, the process can be sped up to 10 times the normal rate. These cells cannot be shed rapidly enough, so they build up on the surface, leading to the think, dry patches that are the hallmark of plaque psoriasis, the most common form of the disease. Redness and inflammation typically accompany the patches of dry skin.
The five distinct types of psoriasis that different people face.
- Plaque Psoriasis
Plaque psoriasis is the most common type of psoriasis and most often appears on the elbows, knees, scalp and back, although it can appear anywhere on the body, including the hands, feet, and genital area. It is often triggered by illness or infection, and is often worse in cold weather, although in many cases it is not possible to determine the cause of an outbreak. One way psoriasis can advance on one’s body is through the Koebner phenomenon, in which skin injury or trauma (or even rough scratching of the skin) can later lead to new spots of psoriasis. - Inverse Psoriasis
Inverse psoriasis (also called flexural psoriasis) typically occurs in moist areas of the body and in the folds of the skin, including under the breasts or armpits and in the genital area. Sweat, friction and body movement can add to the pain and inflammation of inverse psoriasis. It is more common in people who are overweight. It is typically smooth and inflamed, rather than dry and scaly. - Guttate Psoriasis
Guttate psoriasis is a form of the disease that typically comes on rapidly in a flare of teardrop-shaped spots. About 10% of people with psoriasis will develop guttate psoriasis at some point, although it more often appears in children and young adults. It most often follows a strep throat infection. - Pustular Psoriasis
This uncommon form of psoriasis usually appears on the hands and feet, with pus-filled sores that resemble blisters. But it can also be a widespread flare that can be life-threatening. One reason to avoid “cold turkey” quitting of corticosteroids like prednisone is because it can trigger a flare of pustular psoriasis, even in a person with plaque psoriasis. That is why your physician will typically tell you to wean off steroids, rather than quit abruptly. - Erythrodermic Psoriasis
Erythrodermic psoriasis is a rare, severe and dangerous form of the disease. It usually entails widespread coverage with inflamed areas of skin that are red and painful, and giving off heat. Erythrodermic psoriasis requires prompt medical attention.

Psoriasis and psoriatic arthritis can—and should—be treated. Undertreatment of psoriasis appears to be a real problem, but treatment options for patients continue to expand and improve. Please read more about the exciting new breakthroughs in psoriasis treatment options. And if you have other than plaque psoriasis, be sure to check out Treatments for Inverse, Guttate, Pustular, & Erythrodermic Psoriasis. It’s time for all psoriasis patients to benefit from the wonders of science and medicine.
[Last updated 5-25-2019]


